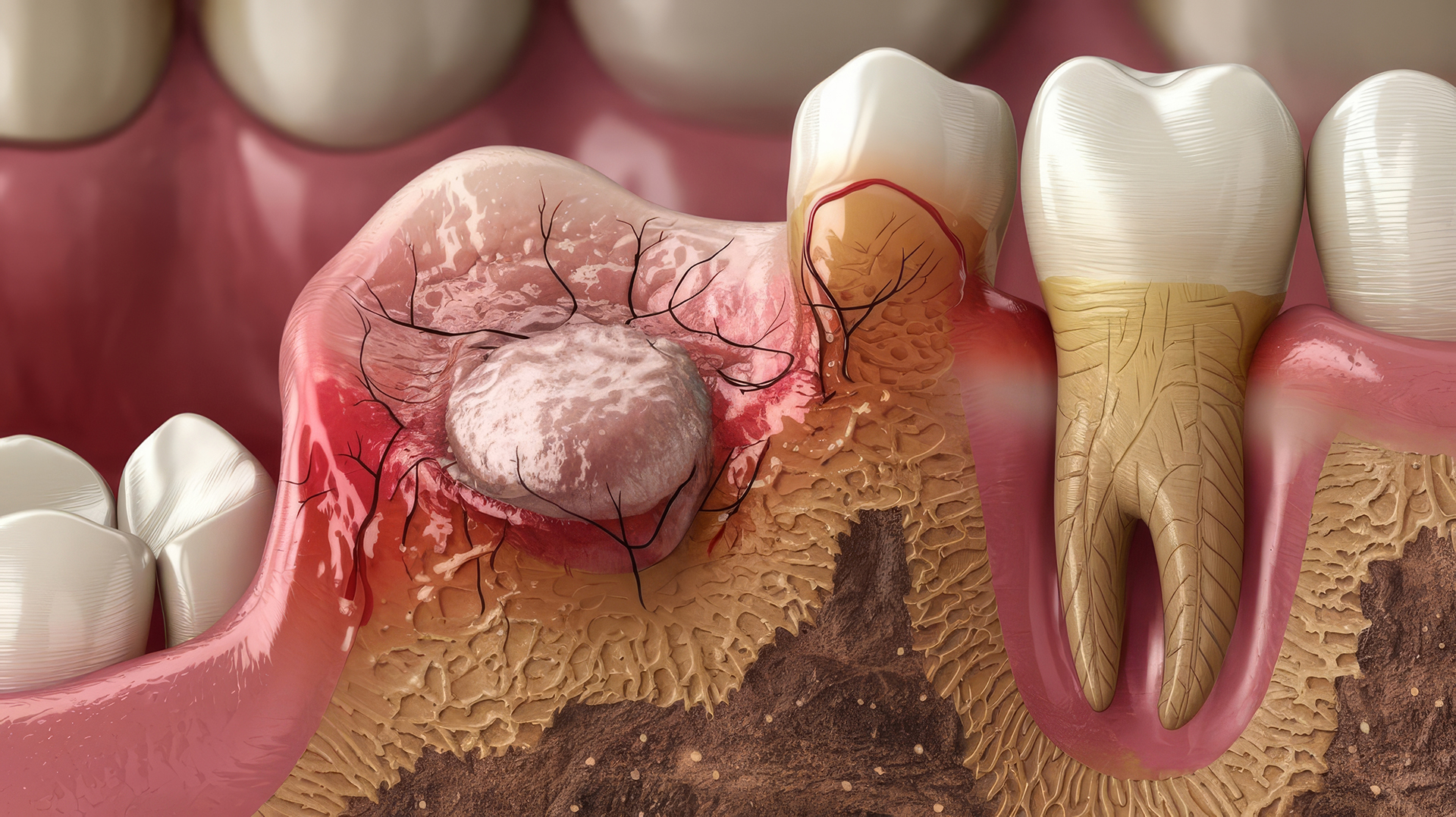
A dental abscess is a pocket of pus caused by a bacterial infection inside or around a tooth. It is not something that goes away on its own — and unlike most dental issues, it can become genuinely dangerous if left untreated. The infection can spread from the tooth into the surrounding bone, the jaw, the neck, and in severe cases, into the bloodstream — a life-threatening condition known as sepsis.
The good news is that with prompt dental treatment, an abscess can be resolved effectively and the tooth can often be saved. The key word is prompt. If you suspect you have an abscessed tooth, this is not a situation to wait and see.
Types of Dental Abscesses
Not all abscesses are the same. Understanding the type helps explain why certain treatments are recommended.
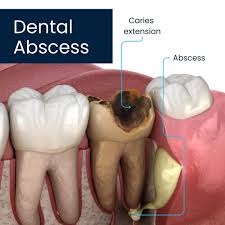
Periapical abscess This is the most common type. It forms at the tip of the tooth root, usually as a result of untreated tooth decay that has reached the inner pulp of the tooth. Bacteria infect the pulp tissue, and the infection spreads downward through the root into the surrounding bone.
Periodontal abscess This type develops in the gum tissue alongside the tooth, often as a result of advanced gum disease. It does not always involve the tooth’s inner pulp and is more related to the supporting structures around the tooth.
Pericoronitis A localized infection around a partially erupted tooth — most often a wisdom tooth — where bacteria become trapped under a flap of gum tissue.
Warning Signs You Should Not Ignore
Dental abscesses can develop gradually, but they often announce themselves clearly. Seek dental care immediately if you experience any of the following:
- Severe, persistent toothache that throbs and may radiate to the jaw, neck, or ear
- Swelling in the face, cheek, or jaw
- Sensitivity to hot and cold that lingers well after the source is removed
- Pain when biting or chewing
- Fever and general feeling of being unwell
- A visible pimple-like bump on the gum near the affected tooth
- Swollen, tender lymph nodes under the jaw or neck
- A sudden rush of foul-tasting, salty fluid in the mouth — which may indicate the abscess has burst
If you have facial swelling combined with difficulty breathing or swallowing, go to the emergency room immediately. This indicates the infection may be spreading toward the airway.
How Is a Dental Abscess Treated?
No home remedy eliminates a dental abscess. Treatment must be performed by a dentist, and the goal is always the same: to drain the infection and eliminate its source. Depending on the severity and type of abscess, your dentist will recommend one of the following:
Incision and drainage. For a localised abscess, your dentist will make a small cut in the swollen gum tissue to drain the pus and relieve pressure. The area is then rinsed with saline solution. This provides immediate relief but is typically followed by further treatment to address the source of the infection.
Root canal treatment. If the infection originates inside the tooth, a root canal is usually the preferred treatment. The infected pulp is removed, the inside of the tooth is cleaned and disinfected, and the tooth is sealed and capped with a crown. This eliminates the infection while preserving the natural tooth.
Tooth extraction: If the tooth is too severely damaged to be saved, extraction may be necessary. Removing the tooth eliminates the source of infection. A dental implant or bridge can later replace the missing tooth once the area has fully healed.
Antibiotics: Antibiotics alone cannot cure a dental abscess — they do not penetrate the infected tissue effectively enough to eliminate the infection at its source. However, your dentist may prescribe them alongside dental treatment if the infection has spread beyond the tooth, if you have a fever, or if you are immunocompromised. They are a supporting measure, not a standalone solution.
What You Can Do Before Your Appointment
If you cannot get to a dentist immediately, these measures can help manage discomfort in the meantime — but they are not substitutes for professional treatment:
- Rinse gently with warm salt water several times a day to help draw out some of the infection and soothe the area
- Take over-the-counter pain relief such as ibuprofen, which also helps reduce inflammation
- Avoid very hot, cold, or hard foods that aggravate the affected tooth
- Sleep with your head slightly elevated to reduce throbbing pressure
- Do not apply heat to the outside of your face — it can encourage the infection to spread
Contact your dentist the same day or go to an emergency dental clinic. Most practices keep time available for dental emergencies, exactly for situations like this.
How to Prevent a Dental Abscess
Most abscesses are the result of untreated tooth decay or advanced gum disease — both of which are largely preventable with consistent care:
- Brush twice daily with a fluoride toothpaste and floss once a day
- Attend regular dental checkups and professional cleanings every six months
- Address cavities and gum disease early, before they progress to deeper infection
- Avoid sugary foods and drinks that accelerate decay
- Wear a mouthguard if you grind your teeth, as grinding can crack teeth and create entry points for bacteria
Frequently Asked Questions
1. Can a dental abscess go away on its own?
No. A dental abscess will not resolve without professional treatment. It may appear to improve temporarily if the abscess bursts and drains on its own, but the underlying infection remains. Without treatment, it will return — and likely worsen. The source of the infection must be addressed by a dentist.
2. How quickly can a dental abscess become dangerous?
It varies, but an untreated abscess can spread to surrounding tissues within days. If swelling begins to affect your jaw, neck, or if you develop a fever and difficulty swallowing, seek emergency care immediately — these are signs the infection is spreading beyond the tooth.
3. Will the dentist pull the tooth if I have an abscess?
Not necessarily. Extraction is one option, but many abscessed teeth can be saved with a root canal. Your dentist will assess the extent of the damage and recommend the most conservative treatment that effectively eliminates the infection.
4. Is it safe to take antibiotics and skip the dental visit?
No. Antibiotics can temporarily reduce symptoms and slow the spread of infection, but they cannot eliminate the source. The abscess will return once the course of antibiotics ends. Dental treatment is always required to fully resolve the infection.
“A dental abscess is one of the few dental conditions where waiting even a day or two can make a real difference in your outcome — if you’re in pain or notice swelling, call us immediately and we will make time for you the same day.”